|
PICC lines should be cleansed and dressed. The initial IV is then split apart leaving the PICC line alone remaining in the vein. The PICC catheter is then placed through the IV which is already in the vein and advanced until the tip is near the heart. The PICC line is trimmed to a length that will allow the tip to lie near, but not in the heart. A special plastic IV catheter, which can be split apart and which is large enough to admit the PICC line itself, is placed into a vein. PICC lines commonly are available in sizes from 2 French to 7 French (3 French = 1 mm). I think some PICC catheters are cut to length which is why they must be measured on removal.I am familiar with the broviac I am confused by the way you have written some of your questions so hope the above helps a bit. Can't tell you the amount of times I've seen peopel inject into a PICC without swabbing it first with alcohol. Maintain strict cleanliness with PICC lines as the patient can pick up infections very easily from dirty hands and unsterile techniques. What do you mean all meds come out the tip of the PICC? I for one am a bit confused by your questions. PICCs can be used for nutritional reasons too and are very versatile. These can be labelled, but usually aren't. Red could be to draw blood, blue for IV medications, another port, ie: white, could be used for chemotherapy. They can thread PICCs thru any large vein if necessary though.Īll PICC lines I have used have multiple ports that are usually coloured. The PICC line needs to stay intact as medications go right into the patients superior vena cava, to their heart & circulatory system. I don't know why u think we would need to cut the tip or the port? What rationale did you have in mind for that - just interested in your thinking process. People from other countries may have different ways of saying things too. OP you are shooting yourself in the foot as we can't understand what your abbreviations are and therefore you may lose out on valuable answers. This suggests 16-cm triple-lumen CVCs can be used safely.What is an EHR? What does TLC stand for? Sorry can people PLEASE put the full word at first, then the abbreviation in brackets. 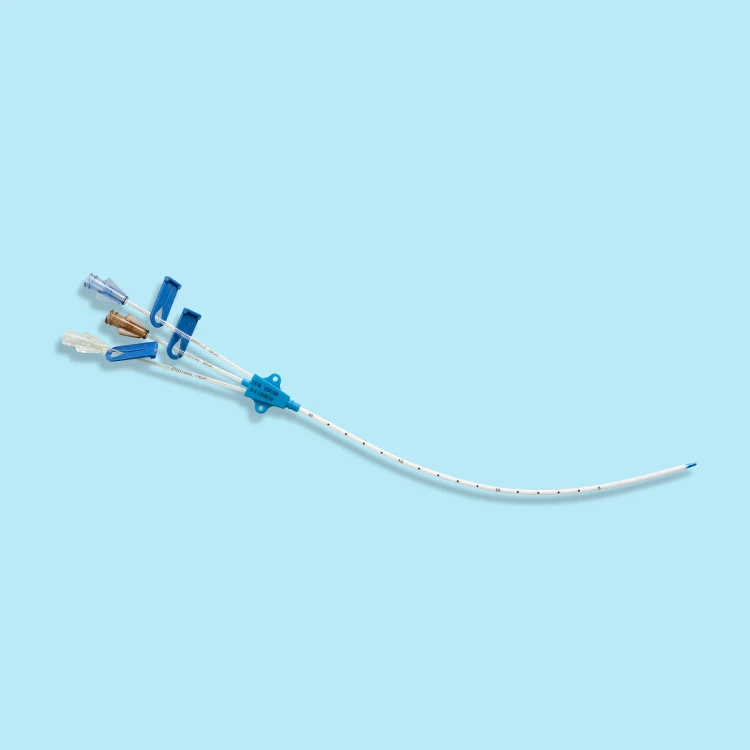
No CVCs failed under dynamic loading with injection of contrast at flow rates (4.5 and 7 mL/s) high enough to support computed tomographic angiography. During dynamic testing the mean peak pressures at 7 mL/s was 81.1 PSI (95% CI 73-89.2 PSI). PSI at burst during static testing was 184.2 PSI (95% confidence interval 174.3-194.1 PSI). Pressures were recorded throughout injection.ĭuring static testing, 6/7 CVCs burst at the distal lumen where the glue was applied, the remaining CVC burst proximal to the hub.   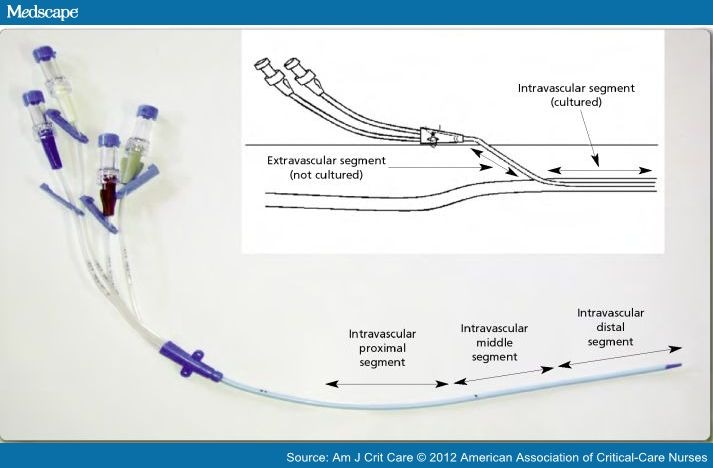
Dynamic pressure testing was done with the remaining catheters, with radio-contrast injected through the unoccluded distal lumen at flow rates of 4.5 mL/s, then 7 mL/s. The CVC was then placed into a 10-cm deep water bath at 37☌ to simulate in vivo conditions and water was injected until catheter rupture. Half the CVCs (n = 7) were subjected to static testing, where the distal lumen was occluded with the guidewire and super glue at the distal end of the catheter. We gathered 16-cm long triple-lumen CVCs (n = 14) from patients with an average dwell time of 5.2 days (☒.7 days). The CVC might rupture at high flow rates, resulting in CVC fragmentation and embolization or contrast extravasation.The objective of this study is to determine the pressure required to burst a CVC under static load and compare this to the pressure generated by injection of contrast at high flow rates (dynamic load) through the distal (16-g) lumen of a triple-lumen CVC. Patients undergoing computed tomographic angiography require injection of contrast at high flow rates (4.5 mL/s), often CVC access is not used due to safety concerns. Central venous catheter (CVC) access is commonplace in intensive care units.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
